BME for Global Health
Biomedical Engineering for Sustainable Global Health: PhD Scholarships
Objectives
Health systems are facing complex local (e.g. demographic change, population ageing, sandwich generation) and global challenges (e.g. international health emergencies, antimicrobial resistance, pandemics, climate change, wars, global warming), which led the WHO to introduce in the Strategic Plan 2025-2028 new priorities such as the development of climate-resilient health systems and lowering carbon footprint of health systems and societies. There are several factors pushing this shift into WHO priorities. For instance, in 2024 potential carriers of vector of Nila Virus, Zika and Malaria were found respectively in Canada, Scotland and Italy. Moreover, European healthcare systems are responsible for the 5% of Co2 EU emissions, which is remarkable (e.g., transports account “only” for 15%). As a proxy for demographic changes, a report from a world leading medical device manufacturer estimated that by 2040 one fourth of the European population should work for the healthcare system, to balance the growing request of care due to aging population. This urges the provision of innovative technologies that can protect healthcare workers and free their time from repetitive routinary activities, leveraging on key enabling technologies such as robots, AI, and IoT.
To address these challenges, it is necessary to rethink the organization of health services for the well-being of people and the communities in which they live. To be effective, biomedical engineering need to work side-by-side with experts of sustainability and strength their collaborations with experts of global health, which are the once in charge for the reorganization of healthcare services in most countries. In fact, the conscious use of enabling and transformative technologies can provide safe, effective, and efficient solutions, while simultaneously generating new knowledge and new opportunities for sustainable economic development, in line with the UN SDGs. However, the adoption of innovative technologies is effective and sustainable, as well as safe and efficient, if and only if it is accompanied by an actual reorganization of services. Our community is requested to put global effort in finding innovative and sustainable technological solutions, which may help transforming healthcare systems, following the United Nations Sustainable Development Goals 2030 (SDG2030) and in line with the 5As principles: affordability, availability, accessibility, accommodation, and acceptability.
This project aims at fostering the growth of biomedical engineering for sustainable global health via PhD scholarship, open also to candidates from LMICs, which are willing to depp dive into this systematic change.
Health systems are facing complex local (e.g. demographic change, population ageing, sandwich generation) and global challenges (e.g. international health emergencies, antimicrobial resistance, pandemics, climate change, wars, global warming), which led the WHO to introduce in the Strategic Plan 2025-2028 new priorities such as the development of climate-resilient health systems and lowering carbon footprint of health systems and societies. There are several factors pushing this shift into WHO priorities. For instance, in 2024 potential carriers of vector of Nila Virus, Zika and Malaria were found respectively in Canada, Scotland and Italy. Moreover, European healthcare systems are responsible for the 5% of Co2 EU emissions, which is remarkable (e.g., transports account “only” for 15%). As a proxy for demographic changes, a report from a world leading medical device manufacturer estimated that by 2040 one fourth of the European population should work for the healthcare system, to balance the growing request of care due to aging population. This urges the provision of innovative technologies that can protect healthcare workers and free their time from repetitive routinary activities, leveraging on key enabling technologies such as robots, AI, and IoT.
To address these challenges, it is necessary to rethink the organization of health services for the well-being of people and the communities in which they live. To be effective, biomedical engineering need to work side-by-side with experts of sustainability and strength their collaborations with experts of global health, which are the once in charge for the reorganization of healthcare services in most countries. In fact, the conscious use of enabling and transformative technologies can provide safe, effective, and efficient solutions, while simultaneously generating new knowledge and new opportunities for sustainable economic development, in line with the UN SDGs. However, the adoption of innovative technologies is effective and sustainable, as well as safe and efficient, if and only if it is accompanied by an actual reorganization of services. Our community is requested to put global effort in finding innovative and sustainable technological solutions, which may help transforming healthcare systems, following the United Nations Sustainable Development Goals 2030 (SDG2030) and in line with the 5As principles: affordability, availability, accessibility, accommodation, and acceptability.
This project aims at fostering the growth of biomedical engineering for sustainable global health via PhD scholarship, open also to candidates from LMICs, which are willing to depp dive into this systematic change.
Support
This project is supported by foundations (e.g., Med’Or), EU projects (such as GATEKEEPER, ODIN, EPoCA, Enkore) and National Research grants (e.g., Afya Moja, “One Health” in Swahili) aiming at bridging research and global health ecosystems across different phases of medical devices lifecycle in which BME are involved: design, manufacturing, clinical and pre-clinical validation, regulations, assessment and management.
Case Studies and Projects
Click to open single project
Innovative health technologies for low-resource settings
A vest for treating jaundice in low-resource settings
Neonatal jaundice (NJ) is one of the most common conditions in newborns (60-80% births, with 10% requiring treatment), the 7th cause of neonatal mortality, with a significant health burden for LMICs. NJ is usually due to the incapacity of neonatal livers to metabolize unconjugated bilirubin as they are still organically developing. It results in yellow coloration of the skin and sclera because of the accumulation of conjugated or unconjugated bilirubin. In higher income countries, where babies are born in hospital, NJ is treated with blue light while in the incubator.
In LMICs, most of births happens at home and newborns develop skin pigmentation within 5-7 days, which make light therapy ineffective.
This is why we developed the NJ vest. Read more here: A vest for treating jaundice in low-resource settings

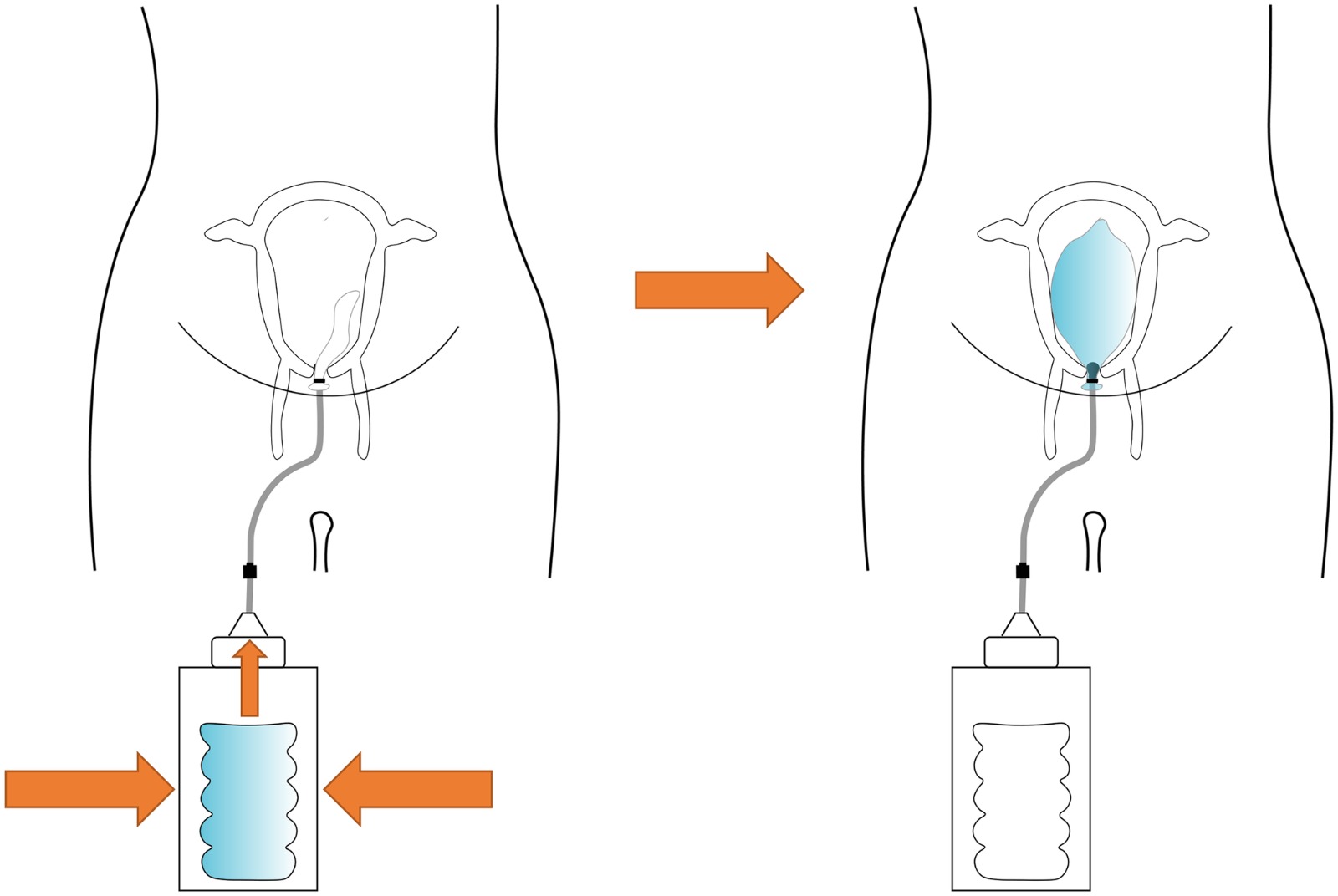
A 3D-printed condom intrauterine balloon tamponade: Design, prototyping, and technical validation
Post-partum haemorrhage is among the main causes of (preventable) mortality for women in low-resource settings (LRSs), where, in 2017, the mortality ratio was 462 out of every 100 000 live births, over 10 times higher than for high-resource settings. There are different treatments available for post-partum haemorrhage. The intrauterine balloon tamponade is a medical device that proved to be a simple and cost-effective approach. Currently, there are several balloon tamponades available, with different design and working principles. However, all these devices were designed for high-resource settings, presenting several aspects that could be inappropriate for many lower-income countries. This paper presents the results of a preclinical study aiming at informing the design, prototyping and validation of a 3D-printed intrauterine balloon tamponade concept, contributing towards the United Nation’s Sustainable Development Goal 3: Good health and Well-being. Frugal engineering concepts and contextualised design techniques were applied throughout, to define the design requirements and specifications. The performance of the final prototype was validated against the requirements of the UK National Health System (NHS) technical guidelines and relevant literature, measuring the water leak and pressure drop over time, both open air and in a approximate uterus model. The resulting prototype is made up of six components, some of which are easy to retrieve, namely a water bottle, a silicone tube and an ordinary condom, while others can be manufactured locally using 3D printers, namely a modified bottle cap, a flow stopper and a valve for holding the condom in place. Validation testing bore promising results with no water or pressure leak open air, and minimal leaks in the approximate uterus model. This demonstrates that the 3D printed condom-based intrauterine balloon tamponade is performing well against the requirements and, when compared to the state of the art, it could be a more appropriate and more resilient solution to low-resource settings, as it bypasses the challenges in the supply of consumables and presents a greener option based on circular economy.
Read more here: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0303844
AI-powered mobile phones as a diagnostic tool
Screening diabetic neuropathies
Objective
Diabetes is a chronic disease characterized by high blood glucose levels, caused by insufficient insulin production or the body’s reduced ability to use it effectively. If not properly managed, diabetes can lead to severe complications, including diabetic neuropathies. This condition manifests as a progressive loss of sensation, particularly in the lower limbs, increasing the risk of ulcers and infections. In severe cases, these lesions may lead to amputations, significantly impacting patients’ quality of life. The issue is particularly relevant in African regions, where diabetes prevalence is high due to inadequate lifestyles and limited access to healthcare.
The proposed solution transforms a mobile phone into an advanced diagnostic device through a dedicated app and two 3D-printed accessories. The first accessory, a small rounded spur, focuses the phone’s vibration on a specific body point, mimicking traditional tools such as tuning forks to assess vibratory sensitivity. The second accessory measures skin sensitivity resolution using two progressively closer-together tips, providing accurate data on neuropathy progression. Thanks to this innovation, non-specialist healthcare workers can perform reliable diagnostic assessments, overcoming the shortage of medical specialists that affects many areas of the continent.
The project is strongly aligned with the United Nations’ 2030 Agenda, particularly Sustainable Development Goal 3, which focuses on health and well-being and aims to reduce diabetes-related mortality. Additionally, it fits within the context of the Fourth Industrial Revolution in healthcare, promoting the use of advanced technologies to improve disease management.
Status
The project is currently ongoing, as a field evaluation of the smart tool is required.
Next steps
Currently, the project is awaiting the necessary ethical approval to initiate the experimental trials.
Country of reference
The project was designed with a specific focus on the South African context, considering the region’s healthcare needs and the challenges related to resource availability.
References
Davide Piaggio, Rossana Castaldo, Gianluca Garibizzo, Ernesto Iadanza, Leandro Pecchia,
A smartphone-based tool for screening diabetic neuropathies: A mHealth and 3D printing approach, Biomedical Signal Processing and Control, Volume 89, 2024, 105807, ISSN 1746-8094, https://doi.org/10.1016/j.bspc.2023.105807
Read more here: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0303844

Diagnosis of pediatric pneumonia
Objective
The present study aims to develop an intelligent tool to support the diagnosis of bronchitis and pneumonia in resource-limited settings. For this reason, an artificial intelligence-based app was designed to analyze easily measurable symptoms without the need for advanced diagnostic tests, which are often unavailable in these areas. Distinguishing pneumonia from other respiratory diseases, such as bronchitis, is a significant challenge. To address this problem, data from 4,500 patients were analyzed and three different artificial intelligence models were tested. The developed algorithm assesses the presence and degree of severity of six key symptoms, providing accuracy and sensitivity exceeding 90 percent. The methodology does not require the use of biological samples, thus eliminating the need for specialized laboratories and reducing the risk of infection. Due to its ease of use, this app provides an affordable solution to improve diagnosis and management of patients in resource-limited settings.
Status
the project has been suspended due to the Covid-19 pandemic
Next steps
the project is waiting for ethical approval
Country of reference
the project is designed for application in countries on the African continent, particularly the state of Benin
Reference:
Stokes, K., Castaldo, R… & Pecchia, L. (2021). A machine learning model for supporting symptom-based referral and diagnosis of bronchitis and pneumonia in limited resource settings. Biocybernetics and biomedical engineering, 41(4), 1288-1302. https://doi.org/10.1016/j.bbe.2021.09.002
Assessment of head trauma through ocular reflex analysis
Objective
The Oida project was created to address an urgent issue in countries like Nigeria, where road accidents are among the leading causes of death due to the exponential growth of traffic on often inadequate infrastructure. In such cases, quickly identifying a cranial trauma can mean the difference between life and death. However, in remote or under-resourced healthcare centers, advanced diagnostic tools and specialized medical personnel are often lacking.
Oida is an Android smartphone app that uses the phone’s flash to analyze the pupillary reflex. The flash triggers pupil constriction, and the AI evaluates the subsequent dilation by analyzing regularity, symmetry, and response times. This allows for real-time exclusion of cranial trauma, providing a valuable tool for rapid triage and timely referral of the patient to the most appropriate treatment.
Status
The app is already in an advanced development stage: it has been successfully tested and has outperformed much more expensive medical devices.
Next Steps
App testing and on-site trials. Improvement of app usability for healthcare workers, as well as enhanced compatibility with different smartphone models and adaptability to all types of eyes.
Country of reference
The project is designed for settings with limited infrastructure, such as many areas in Nigeria. It follows WHO principles to ensure that it is accessible, easy to use, robust, and well-suited to local conditions.
Reference
Piaggio D. et al. (2021). Pupillometry via smartphone for low-resource settings, Biocybernetics and Biomedical Engineering. https://doi.org/10.1016/j.bbe.2021.05.012

Technology and cooperation for One Health in Africa
Enhancing surveillance and interventions for vector control in sub-Saharan Africa
Objective:
In West Africa, technology is stepping in to fight malaria, dengue, and Zika. In Benin, an innovative project aims to develop a “smart trap”: a high-tech device capable of recognizing mosquitoes, identifying their species, and analyzing the viruses they carry.Equipped with sensors, cameras, and genetic analysis tools, the smart trap will collect valuable data directly in the field and transmit it in real time to a digital platform. It’s a new and precise weapon in the fight against vector-borne diseases: fewer insecticides, more targeted interventions, and greater safety for people and the environment. The goal is ambitious but clear: to stop outbreaks before they even begin.
State of Project
Ongoing (Design and prototype development)
Country of reference
Benin
Next steps
Prototype development and testing; On-site field trial (A collaboration is being finalized with the University of Benin to support a master’s thesis in Biomedical Engineering, allowing a graduate student from Campus Bio-Medico to contribute to the local prototype testing.)
Reference:
• A systematic literature review titled “The Point on Mosquito Surveillance Systems: A Scoping Review of Technological Advances over the Past Decade“, currently submitted to BMJ Global Health, analyzing the main technological advancements in mosquito surveillance systems over the last ten years.

Circular health and sustainability
Design and maintenance of medical oxygen concentrators in Sub-Saharan Africa
Objective
The objective of this project is to explore methods for recycling exhausted zeolite, a key material used in portable oxygen concentrators, which are medical devices that generate oxygen for patients. The aim is to develop sustainable solutions for reusing or regenerating zeolite, extending the lifespan of these devices and reducing their costs., This could make oxygen therapy more accessible, especially in low-resource settings, ultimately improving healthcare.
Status
By collecting and characterizing samples from different African countries, we identified the factors that influence and limit the functionality of zeolites in low-resource environments. This helped to refine the mechanism of reuse. We’re just finishing up the regeneration process and preparing it for validation in the lab with newly collected zeolite samples.
Next steps
Verify the results with our established laboratory methods and evaluate the effect of moisture with the help of a simulated system developed in the laboratory.
Country of reference
Sub saharian countries (Sud Africa, Uganda, Ethiopia)
References
1. Ibrahim, N.H., Wallace, J., Piaggio, D. et al. Validation of a framework for assessing healthcare facilities in low-resource settings: a field study in selected facilities in Ethiopia. Health Technol. 15, 201–209 (2025). https://doi.org/10.1007/s12553-025-00943-1
2. Ibrahim, N.H., Wallace, J., Piaggio, D. et al. Design and maintenance of medical oxygen concentrators in Sub-Saharan Africa: a systematic review. BMC Health Serv Res 25, 171 (2025). https://doi.org/10.1186/s12913-025-12315-6
3. Mazzeo, L., Ibrahim, N.H., Pickering, K.S. et al. Understanding oxygen concentrator failures in low resource settings: the role of dust and humidity. Appl Sci 15, 4311 (2025). https://doi.org/10.3390/app15084311.
Projects
EPoCA
Objective:
The ongoing Ebola outbreaks in the Democratic Republic of Congo underscore the urgency of acting in Ebola-endemic regions, focusing on early diagnosis, mitigation and strengthening health systems.
In this respect, the EPoCA project aims to develop and test an innovative device capable of performing rapid and remote diagnosis of Ebola infection. Based on a graphene sensor, an abundant and easily available material, unlike the rare earths used in other sensors, the device will be able to perform the diagnosis directly on site, even in rural areas, without the need for equipped laboratories or specialized personnel. A drop of blood will be enough to simultaneously measure several parameters that, compared and combined with each other through artificial intelligence (AI) methods, will allow to generate a “fingerprint” of the infection. This will not only determine whether a subject is infected but will also allow to quantify the severity of the infection or any mutations of the virus, ensuring diagnostic accuracy.
Finally, the result will be transmitted digitally to a central server that processes the data through AI software and communicates in real time with the WHO, automatically identifying any epidemic outbreaks and allowing health authorities to intervene quickly.
AI will therefore be a fundamental epidemiological surveillance tool, in territories where every hour counts. If a new epidemic were to ever explode, we want the information to arrive before the virus.
Status
Addressing regulatory and ethical aspects
Country of reference
Republic of the Congo, Ghana
Next steps
Design and development of the Point of Care platform
Reference:
https://iht.unicampus.it/epoca/
Case Studies and Projects
Click to open single project
Innovative health technologies for low-resource settings
A vest for treating jaundice in low-resource settings
Neonatal jaundice (NJ) is one of the most common conditions in newborns (60-80% births, with 10% requiring treatment), the 7th cause of neonatal mortality, with a significant health burden for LMICs. NJ is usually due to the incapacity of neonatal livers to metabolize unconjugated bilirubin as they are still organically developing. It results in yellow coloration of the skin and sclera because of the accumulation of conjugated or unconjugated bilirubin. In higher income countries, where babies are born in hospital, NJ is treated with blue light while in the incubator.
In LMICs, most of births happens at home and newborns develop skin pigmentation within 5-7 days, which make light therapy ineffective.
This is why we developed the NJ vest. Read more here: A vest for treating jaundice in low-resource settings

A 3D-printed condom intrauterine balloon tamponade: Design, prototyping, and technical validation
Post-partum haemorrhage is among the main causes of (preventable) mortality for women in low-resource settings (LRSs), where, in 2017, the mortality ratio was 462 out of every 100 000 live births, over 10 times higher than for high-resource settings. There are different treatments available for post-partum haemorrhage. The intrauterine balloon tamponade is a medical device that proved to be a simple and cost-effective approach. Currently, there are several balloon tamponades available, with different design and working principles. However, all these devices were designed for high-resource settings, presenting several aspects that could be inappropriate for many lower-income countries. This paper presents the results of a preclinical study aiming at informing the design, prototyping and validation of a 3D-printed intrauterine balloon tamponade concept, contributing towards the United Nation’s Sustainable Development Goal 3: Good health and Well-being. Frugal engineering concepts and contextualised design techniques were applied throughout, to define the design requirements and specifications. The performance of the final prototype was validated against the requirements of the UK National Health System (NHS) technical guidelines and relevant literature, measuring the water leak and pressure drop over time, both open air and in a approximate uterus model. The resulting prototype is made up of six components, some of which are easy to retrieve, namely a water bottle, a silicone tube and an ordinary condom, while others can be manufactured locally using 3D printers, namely a modified bottle cap, a flow stopper and a valve for holding the condom in place. Validation testing bore promising results with no water or pressure leak open air, and minimal leaks in the approximate uterus model. This demonstrates that the 3D printed condom-based intrauterine balloon tamponade is performing well against the requirements and, when compared to the state of the art, it could be a more appropriate and more resilient solution to low-resource settings, as it bypasses the challenges in the supply of consumables and presents a greener option based on circular economy.
Read more here: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0303844

AI-powered mobile phones as a diagnostic tool
Screening diabetic neuropathies
Objective
Diabetes is a chronic disease characterized by high blood glucose levels, caused by insufficient insulin production or the body’s reduced ability to use it effectively. If not properly managed, diabetes can lead to severe complications, including diabetic neuropathies. This condition manifests as a progressive loss of sensation, particularly in the lower limbs, increasing the risk of ulcers and infections. In severe cases, these lesions may lead to amputations, significantly impacting patients’ quality of life. The issue is particularly relevant in African regions, where diabetes prevalence is high due to inadequate lifestyles and limited access to healthcare.
The proposed solution transforms a mobile phone into an advanced diagnostic device through a dedicated app and two 3D-printed accessories. The first accessory, a small rounded spur, focuses the phone’s vibration on a specific body point, mimicking traditional tools such as tuning forks to assess vibratory sensitivity. The second accessory measures skin sensitivity resolution using two progressively closer-together tips, providing accurate data on neuropathy progression. Thanks to this innovation, non-specialist healthcare workers can perform reliable diagnostic assessments, overcoming the shortage of medical specialists that affects many areas of the continent.
The project is strongly aligned with the United Nations’ 2030 Agenda, particularly Sustainable Development Goal 3, which focuses on health and well-being and aims to reduce diabetes-related mortality. Additionally, it fits within the context of the Fourth Industrial Revolution in healthcare, promoting the use of advanced technologies to improve disease management.
Status
The project is currently ongoing, as a field evaluation of the smart tool is required.
Next steps
Currently, the project is awaiting the necessary ethical approval to initiate the experimental trials.
Country of reference
The project was designed with a specific focus on the South African context, considering the region’s healthcare needs and the challenges related to resource availability.
References
Davide Piaggio, Rossana Castaldo, Gianluca Garibizzo, Ernesto Iadanza, Leandro Pecchia,
A smartphone-based tool for screening diabetic neuropathies: A mHealth and 3D printing approach, Biomedical Signal Processing and Control, Volume 89, 2024, 105807, ISSN 1746-8094, https://doi.org/10.1016/j.bspc.2023.105807
Read more here: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0303844

Diagnosis of pediatric pneumonia
Objective
The present study aims to develop an intelligent tool to support the diagnosis of bronchitis and pneumonia in resource-limited settings. For this reason, an artificial intelligence-based app was designed to analyze easily measurable symptoms without the need for advanced diagnostic tests, which are often unavailable in these areas. Distinguishing pneumonia from other respiratory diseases, such as bronchitis, is a significant challenge. To address this problem, data from 4,500 patients were analyzed and three different artificial intelligence models were tested. The developed algorithm assesses the presence and degree of severity of six key symptoms, providing accuracy and sensitivity exceeding 90 percent. The methodology does not require the use of biological samples, thus eliminating the need for specialized laboratories and reducing the risk of infection. Due to its ease of use, this app provides an affordable solution to improve diagnosis and management of patients in resource-limited settings.
Status
the project has been suspended due to the Covid-19 pandemic
Next steps
the project is waiting for ethical approval
Country of reference
the project is designed for application in countries on the African continent, particularly the state of Benin
Reference:
Stokes, K., Castaldo, R… & Pecchia, L. (2021). A machine learning model for supporting symptom-based referral and diagnosis of bronchitis and pneumonia in limited resource settings. Biocybernetics and biomedical engineering, 41(4), 1288-1302. https://doi.org/10.1016/j.bbe.2021.09.002

Assessment of head trauma through ocular reflex analysis
Objective
The Oida project was created to address an urgent issue in countries like Nigeria, where road accidents are among the leading causes of death due to the exponential growth of traffic on often inadequate infrastructure. In such cases, quickly identifying a cranial trauma can mean the difference between life and death. However, in remote or under-resourced healthcare centers, advanced diagnostic tools and specialized medical personnel are often lacking.
Oida is an Android smartphone app that uses the phone’s flash to analyze the pupillary reflex. The flash triggers pupil constriction, and the AI evaluates the subsequent dilation by analyzing regularity, symmetry, and response times. This allows for real-time exclusion of cranial trauma, providing a valuable tool for rapid triage and timely referral of the patient to the most appropriate treatment.
Status
The app is already in an advanced development stage: it has been successfully tested and has outperformed much more expensive medical devices.
Next Steps
App testing and on-site trials. Improvement of app usability for healthcare workers, as well as enhanced compatibility with different smartphone models and adaptability to all types of eyes.
Country of reference
The project is designed for settings with limited infrastructure, such as many areas in Nigeria. It follows WHO principles to ensure that it is accessible, easy to use, robust, and well-suited to local conditions.
Reference
Piaggio D. et al. (2021). Pupillometry via smartphone for low-resource settings, Biocybernetics and Biomedical Engineering. https://doi.org/10.1016/j.bbe.2021.05.012

Technology and cooperation for One Health in Africa
Enhancing surveillance and interventions for vector control in sub-Saharan Africa
Objective:
In West Africa, technology is stepping in to fight malaria, dengue, and Zika. In Benin, an innovative project aims to develop a “smart trap”: a high-tech device capable of recognizing mosquitoes, identifying their species, and analyzing the viruses they carry.Equipped with sensors, cameras, and genetic analysis tools, the smart trap will collect valuable data directly in the field and transmit it in real time to a digital platform. It’s a new and precise weapon in the fight against vector-borne diseases: fewer insecticides, more targeted interventions, and greater safety for people and the environment. The goal is ambitious but clear: to stop outbreaks before they even begin.
State of Project
Ongoing (Design and prototype development)
Country of reference
Benin
Next steps
Prototype development and testing; On-site field trial (A collaboration is being finalized with the University of Benin to support a master’s thesis in Biomedical Engineering, allowing a graduate student from Campus Bio-Medico to contribute to the local prototype testing.)
Reference:
• A systematic literature review titled “The Point on Mosquito Surveillance Systems: A Scoping Review of Technological Advances over the Past Decade“, currently submitted to BMJ Global Health, analyzing the main technological advancements in mosquito surveillance systems over the last ten years.

Circular health and sustainability
Design and maintenance of medical oxygen concentrators in Sub-Saharan Africa
Objective
The objective of this project is to explore methods for recycling exhausted zeolite, a key material used in portable oxygen concentrators, which are medical devices that generate oxygen for patients. The aim is to develop sustainable solutions for reusing or regenerating zeolite, extending the lifespan of these devices and reducing their costs., This could make oxygen therapy more accessible, especially in low-resource settings, ultimately improving healthcare.
Status
By collecting and characterizing samples from different African countries, we identified the factors that influence and limit the functionality of zeolites in low-resource environments. This helped to refine the mechanism of reuse. We’re just finishing up the regeneration process and preparing it for validation in the lab with newly collected zeolite samples.
Next steps
Verify the results with our established laboratory methods and evaluate the effect of moisture with the help of a simulated system developed in the laboratory.
Country of reference
Sub saharian countries (Sud Africa, Uganda, Ethiopia)
References
1. Ibrahim, N.H., Wallace, J., Piaggio, D. et al. Validation of a framework for assessing healthcare facilities in low-resource settings: a field study in selected facilities in Ethiopia. Health Technol. 15, 201–209 (2025). https://doi.org/10.1007/s12553-025-00943-1
2. Ibrahim, N.H., Wallace, J., Piaggio, D. et al. Design and maintenance of medical oxygen concentrators in Sub-Saharan Africa: a systematic review. BMC Health Serv Res 25, 171 (2025). https://doi.org/10.1186/s12913-025-12315-6
3. Understanding Oxygen Concentrator Failures in Low Resource Settings: The Role of Dust and Humidity [Under review]
Projects
EPoCA
Objective:
The ongoing Ebola outbreaks in the Democratic Republic of Congo underscore the urgency of acting in Ebola-endemic regions, focusing on early diagnosis, mitigation and strengthening health systems.
In this respect, the EPoCA project aims to develop and test an innovative device capable of performing rapid and remote diagnosis of Ebola infection. Based on a graphene sensor, an abundant and easily available material, unlike the rare earths used in other sensors, the device will be able to perform the diagnosis directly on site, even in rural areas, without the need for equipped laboratories or specialized personnel. A drop of blood will be enough to simultaneously measure several parameters that, compared and combined with each other through artificial intelligence (AI) methods, will allow to generate a “fingerprint” of the infection. This will not only determine whether a subject is infected but will also allow to quantify the severity of the infection or any mutations of the virus, ensuring diagnostic accuracy.
Finally, the result will be transmitted digitally to a central server that processes the data through AI software and communicates in real time with the WHO, automatically identifying any epidemic outbreaks and allowing health authorities to intervene quickly.
AI will therefore be a fundamental epidemiological surveillance tool, in territories where every hour counts. If a new epidemic were to ever explode, we want the information to arrive before the virus.
Status
Addressing regulatory and ethical aspects
Country of reference
Republic of the Congo, Ghana
Next steps
Design and development of the Point of Care platform
Reference:
https://iht.unicampus.it/epoca/

